Michigan No-Fault Medical Providers
Getting Your Hard-Earned Bills Paid
Understand what you need to do to get your No-Fault bills paid.
Getting medical bills paid by a car insurance company is an extremely difficult task in Michigan. If you are a medical provider, it is critical that you fully understand the requirements that must be met in order to receive payment. We discuss the requirements below. Follow these rules to ensure you get paid for your hard work.

You must be able to show that your treatment was related to the accident.
- Physicians, especially surgeons, are often wishy-washy about the source of the injury they are treating. Why? Because, medically, it is often impossible to conclusively state whether an injury was caused by an accident. Accordingly, physicians typically state that injuries could have been caused by the accident. Unfortunately, that statement will not get your bills paid and, in fact, will support the insurer’s denial.
- The plaintiff and providers have the burden of showing the injuries and treatment are related to the accident. If there is doubt as to whether the treatment was necessitated by the accident, the insurer has a good chance to deny the bills and win at trial.
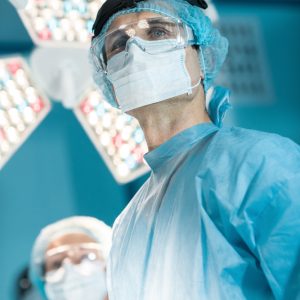
You must be able to show that your treatment was necessary.
- If you are a specialist, a physical therapist, a pharmacist, a home care company, an imaging center, or anyone else that is providing advanced care to a plaintiff, you must have a physician’s script, order, or referral to show that your treatment was necessary.
- With the new Utilization Review that was adopted in 2019 (not yet implemented as of this writing), obtaining a script showing the necessity for a service is even more important than before.
-
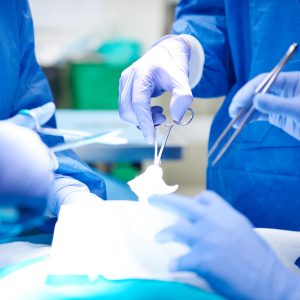
You must be able to show that your treatment was reasonable.
- The reasonableness of a provider’s treatment is always subjective, but there are certain scenarios that are always questionable. A physical therapist cannot continuously provide treatment for two years straight without red flags going off. An MRI facility cannot conduct several MRIs of the cervical spine within a few months. A toxicology laboratory cannot test a patient for the same narcotics several times a month.
- With the new Utilization Review that was adopted in 2019 (not yet implemented as of this writing), the reasonableness of all future procedures will be scrutinized. Accordingly, “pushing the envelope” is not a smart strategy going forward.
-

You must be able to show that your charges are reasonable.
- While most medical provider charges will be capped by the No-Fault fee schedule (MCL 500.3157), those charges that do not have CPT/HCPCS codes covered by Medicare will be subject to a cap of 55% of the provider’s charges. Those charges must be reasonable in order for the payment to be obtained.
- The Fair Health actual value database (fee estimator) is the gold standard in the insurance industry for determining reasonableness. When there is insufficient data to formulate an actual value database, Fair Health maintains a relative value database. Check with the Fair Health database, on the Fair Health website, to determine whether your charges are reasonable.
-
-

Let the top attorneys help you get paid.
For help with collections, billing, utilization review, or provider suits call us at 248-385-5704. You can also email, Pratheep “Seva” Sevanthinathan directly at [email protected]. Mr. Seva has been the leading medical provider attorney in Michigan for the past 15-years. We will get you paid for your hard work.










